About Treatment
Biopsy technology makes it possible to obtain material for research from the most inaccessible body tissues using minimally invasive method.
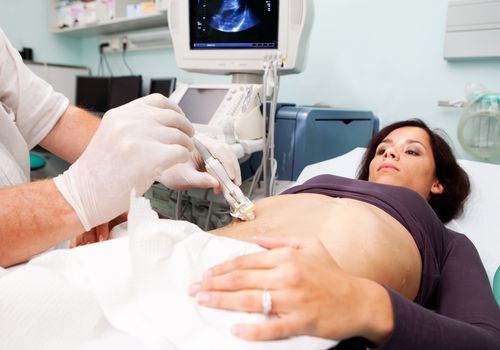
Biopsy is a procedure that allows you to confirm a particular diagnosis by examining the cellular structure of body tissues. The method is indispensable in the diagnosis of cancer. Often, samples for research must be taken from hard-to-reach areas of the body - for example, tissues of internal organs.
If earlier it was necessary to perform an operation for this, now there is no need for this - with the help of new medical technology, tissue samples can be obtained using a minimally invasive method. A special needle is inserted into the affected organ under the control of CT scanner. Thus, cells can be obtained even from a small pathological focus without the risk of damaging adjacent tissues.
The procedure lasts 20 to 30 minutes, including pre-scan, and is done under local anesthetic. Now the department has the opportunity to carry out more than two hundred such procedures per year under the compulsory medical insurance in the direction of a doctor.
How the preocedure is done?
During the procedure, patient lies down, anesthetic drug is injected into the area of the skin puncture. This provides anesthesia for the biopsy site, but does not disturb the subject's consciousness. Then the movable part of the table slides into the scanner. Patient can see and hear staff during entire examination and, if necessary, communicate with doctors.
During the procedure, patient is recommended not to move and hold breath for a short time. At this time, doctor makes puncture of the skin, passes the needle to the planned organ and takes tissue sample.
The needle position is controlled using computer image. After taking the material, the needle is removed.
After biopsy, patient is placed in an observation ward for 4 hours, where the heart is monitored. Patient can then leave hospital.
The extracted piece of tissue is sent to laboratory. At the second consultation, doctor tells patient in detail about the data obtained and explains how they will affect the treatment methods.
What to expect from biopsy?
In general biopsy varies greatly depending on how complex the procedure for obtaining a tissue sample is. In medicine, the term "invasiveness" is used for this.
Minimally invasive biopsy (for example, most skin biopsies) can be done in doctor's office during the same visit that the affected area was found. An anesthetic injection of small dose of drug causes slight numbness of the skin and makes biopsy procedure almost painless.
A more invasive biopsy is done in a hospital, surgery center, or during a visit to a specialist doctor. In most cases, sedatives are also used to help relieve discomfort and pain.
After biopsy, pain in the area where the needle is inserted may be felt for several days. If the pain is severe, your doctor may recommend taking pain relievers.
-
Duration
20-30 minutes
-
Result
5-10 days
It is recommended to have with you results of blood clotting and platelet test; if necessary, they can be repeated;
In the evening before the procedure, do not eat or drink;
First discuss with doctor the procedure for taking medications;
Wear comfortable clothes.
After biopsy is performed, the obtained material is sent for research to laboratory. Research result is usually ready within 5-7 working days.
The biopsy result can have the following interpretations:
Indicative conclusion - diseases are indicated, which include changes in the material under study, but in order to make a final diagnosis, additional diagnostics are required;
Preliminary conclusion - describes the changes in the material under study, so that attending physician, on the basis of this and with a comparison of the results of other studies, makes a final diagnosis;
Final diagnosis - changes in the test material are described in detail and an accurate conclusion on the disease is given. In this case, no further comparisons with the results of other studies are required, and clinical diagnosis is made.
Very often, when suspicious tissue changes, inflammatory processes, tumors or metastases are found, it is difficult to make an exact diagnosis. And here we are talking not only about clinical, but also radiological examinations of patients. In this case, the only way to determine the cause of tissue changes is to take tissue samples under radiological control, and subsequently to examine them under histopathological microscope. CT-guided biopsy is ideal because imaging can not only see changes accurately, but also take samples from a suspicious location with millimeter precision.
CT-guided biopsy is a minimally invasive procedure that is most often performed under local anesthesia and does not cause discomfort to patient. This is undoubtedly an advantage, since during the examination, general anesthesia is not required, and, therefore, does not exert a great load on patient's body. In its complexity, the procedure lasts 20-30 minutes.
The procedure is carried out with great care and accuracy. However, very rarely there are bleeding or damage to neighboring organs, unfortunately, this cannot be 100% avoided. CT-guided biopsy allows for continuous monitoring of the biopsy needle using CT scanner, which reduces the risk of such damage.
After tissue samples are obtained and stored, they are sent for examination to pathologists. A pathologist is a doctor who specializes in diagnosing diseases based on available tissue, cell, and other test results.
Doctor examines the tissue samples under microscope. Peculiarities and types of cells, their shape and internal activity in most cases make it possible to accurately identify the problem. The time during which biopsy result will be ready varies from a few minutes if the pathologist is present during the operation and diagnoses immediately, to a week or more.